Changshan Medical News
Heparin-induced thrombocytopenia (HIT) is a complication characterized by thrombocytopenia caused by heparin, which mainly manifests as thrombocytopenia, platelet activation or thrombosis. There are two clinical types, one is with thrombosis, and the other is only antibody production without thrombosis. The most common type in clinic is the type with thrombosis. Today, I will list two misunderstandings about heparin-induced thrombocytopenia.
Misunderstanding 1: The use of low molecular weight heparin is prone to heparin-induced thrombocytosis.。
Truth 1:The incidence of HIT induced by low molecular weight heparin is far less than that of unfractionated heparin. The HIT induced by unfractionated heparin is the main one, and a few are HIT induced by low molecular weight heparin.
Heparin drug molecules and platelet factor 4 (PF4) form an antigen complex with a chain length of 14 sugar units, which means that heparin molecules with a relative molecular weight of 4200 D or more have the potential to cause HIT, due to low molecular weight heparin The weight average molecular weight of heparin is low, so the incidence of HIT is lower when using low molecular weight heparin than unfractionated heparin. The incidence of low-molecular-weight heparin exposure is 0.1-1%, and the incidence of unfractionated heparin exposure is even higher, about 1-5%. The incidence of surgical patients is higher than that of medical patients.
Misunderstanding 2: The harm of heparin-induced thrombocytopenia is bleeding
Truth 2: The main harm of heparin-induced thrombocytopenia is not bleeding, but thromboembolism.
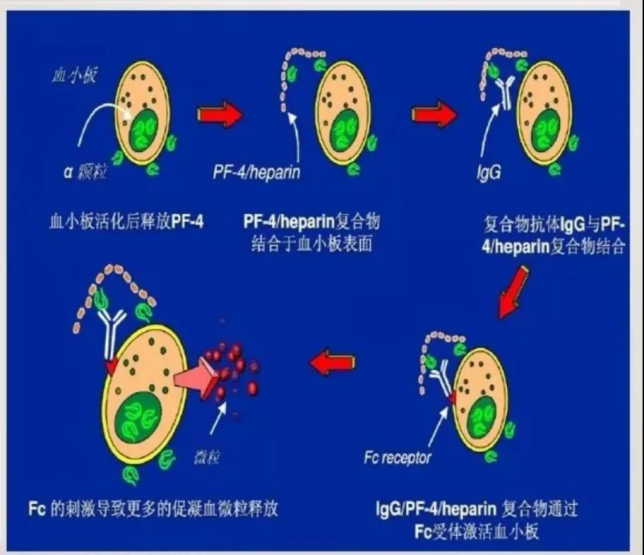
Platelet factor 4 (PF4) is present in the alpha particles in the platelets and is a natural heparin inactivator. Heparin enters the body and combines with platelet factor 4 to form a complex, which induces lymphocytes to produce HIT antibodies. After the antibody is formed, it binds to platelets to activate platelets, binds to endothelial cells to activate endothelial cells, and can also bind to the surface of monocytes to activate monocytes. Endothelial damage activates the coagulation system and platelets. Platelets release microparticles to cause blood hypercoagulation. On the other hand, monocytes release tissue factor to activate the exogenous coagulation system. Therefore, the hazard of heparin-induced thrombocytopenia is thromboembolism. The cause of thrombocytopenia is that platelets are consumed when they aggregate to form a thrombus. In addition, the aggregated platelets are phagocytosed and cleared after binding to endothelial cells and white blood cells, resulting in thrombocytopenia.
Reference: Chinese Expert Consensus on Heparin-induced Thrombocytopenia (2017). Chinese Medical Journal. 2018; 98(6): 408-4
Post time: Jan-31-2021

